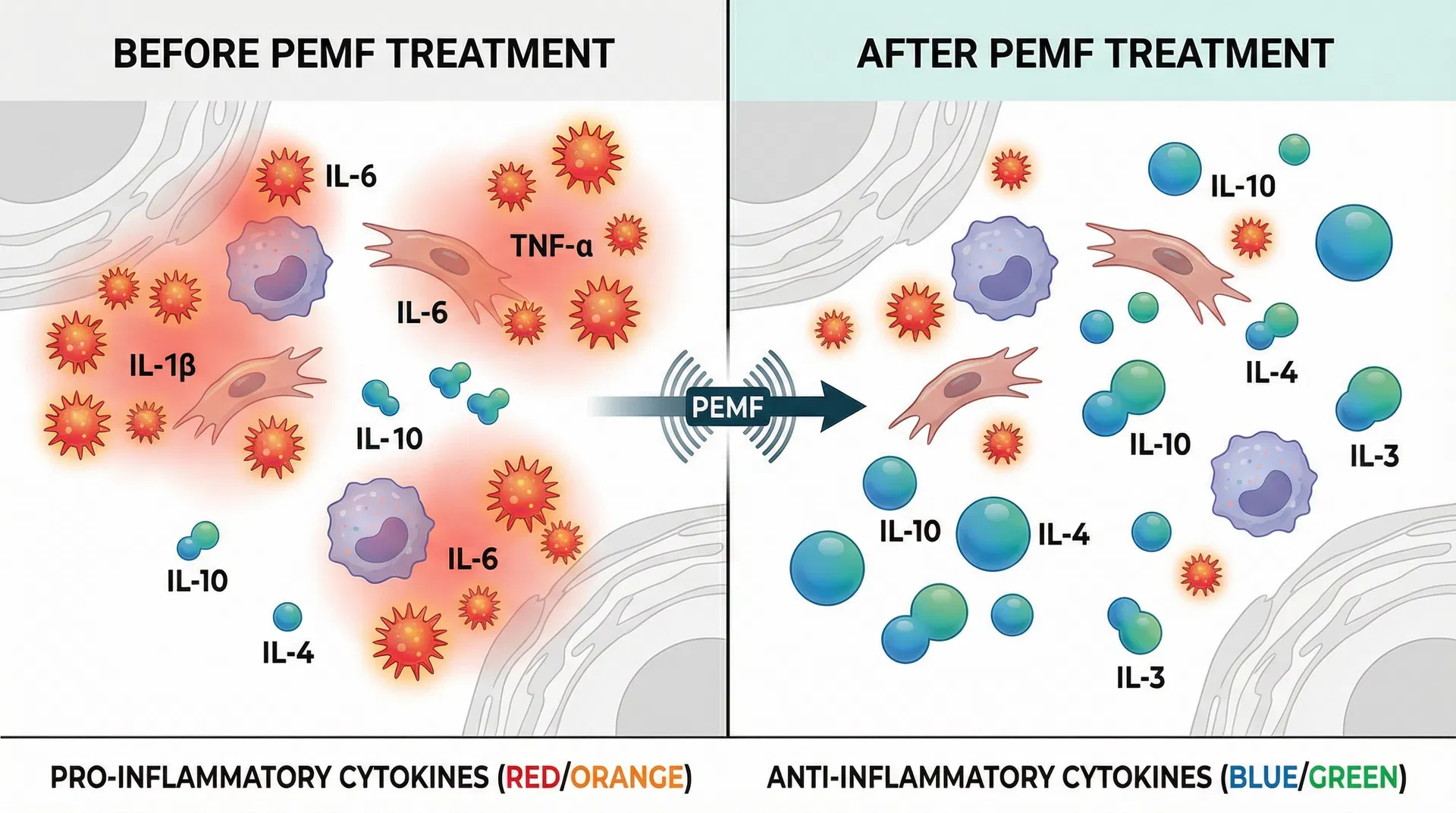
PEMF vs. Traditional Muscle Stimulation: Understanding the Science Behind Different Modalities
Compare PEMF therapy with EMS and TENS techniques. Learn the scientific differences in mechanisms, efficacy, and clinical applications for muscle recovery and healing.

PEMF vs. Traditional Muscle Stimulation: Understanding the Science Behind Different Modalities
Muscle recovery and performance enhancement have become central concerns for athletes, active individuals, and anyone seeking to optimize their physical health. While traditional electrical stimulation techniques like EMS (Electrical Muscle Stimulation) and TENS (Transcutaneous Electrical Nerve Stimulation) have established themselves in rehabilitation and fitness, a newer approach—PEMF (Pulsed Electromagnetic Field) therapy—offers a fundamentally different mechanism for supporting muscle recovery and systemic healing. Our PEMF muscle sculpting treatment harnesses this advanced cellular-level mechanism for superior recovery and body contouring results.
The Fundamental Difference: Where the Action Occurs
The most critical distinction between PEMF and traditional electrical stimulation lies in the level at which each modality operates within the body. This difference shapes everything from immediate effects to long-term outcomes.
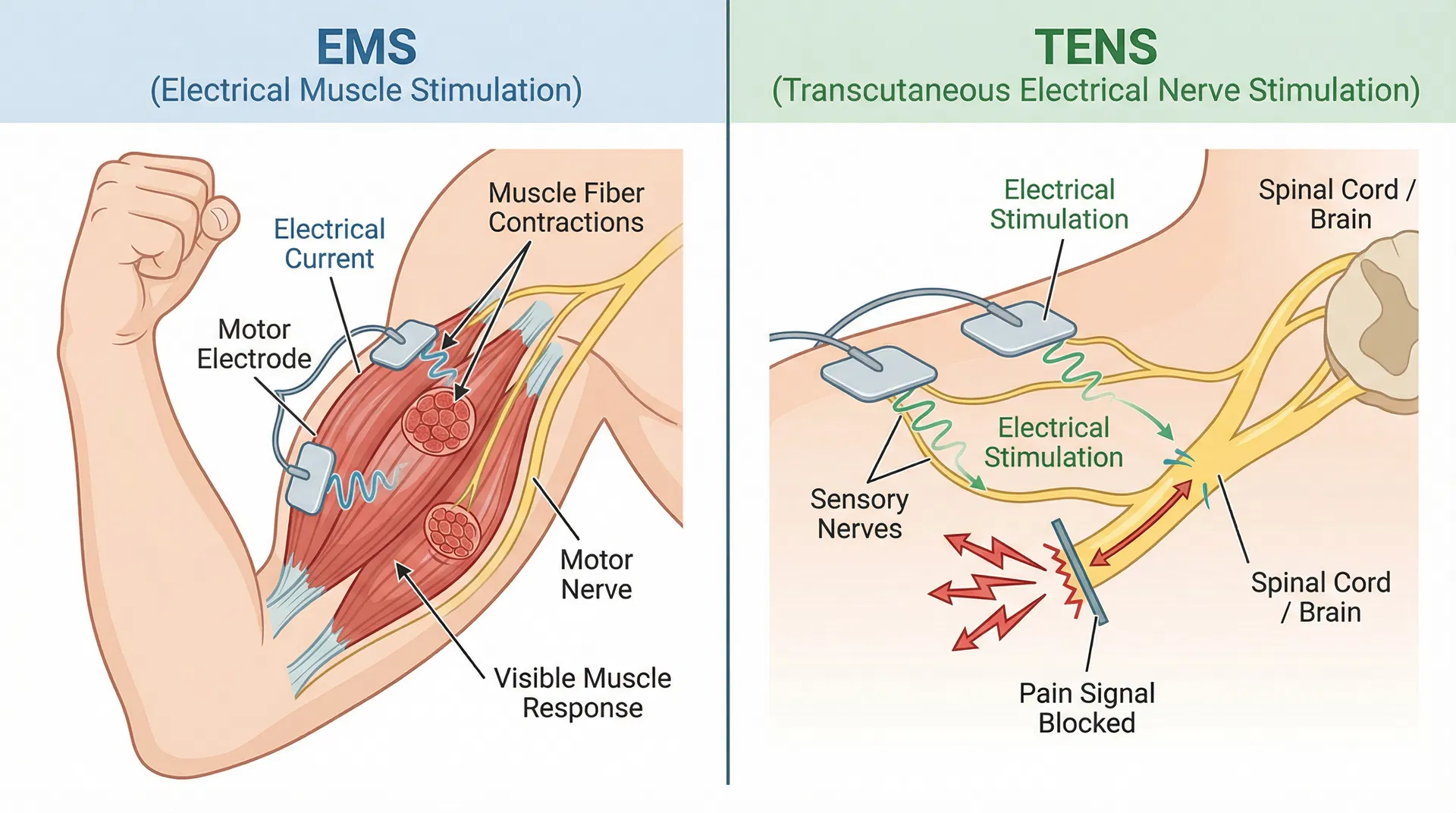
TENS and EMS operate at the nervous and muscular system levels, using electrical current applied directly through electrodes placed on the skin. TENS works by activating sensory nerves, while EMS directly stimulates muscle fibers to produce involuntary contractions. Both are external electrical interventions that create immediate, localized effects.
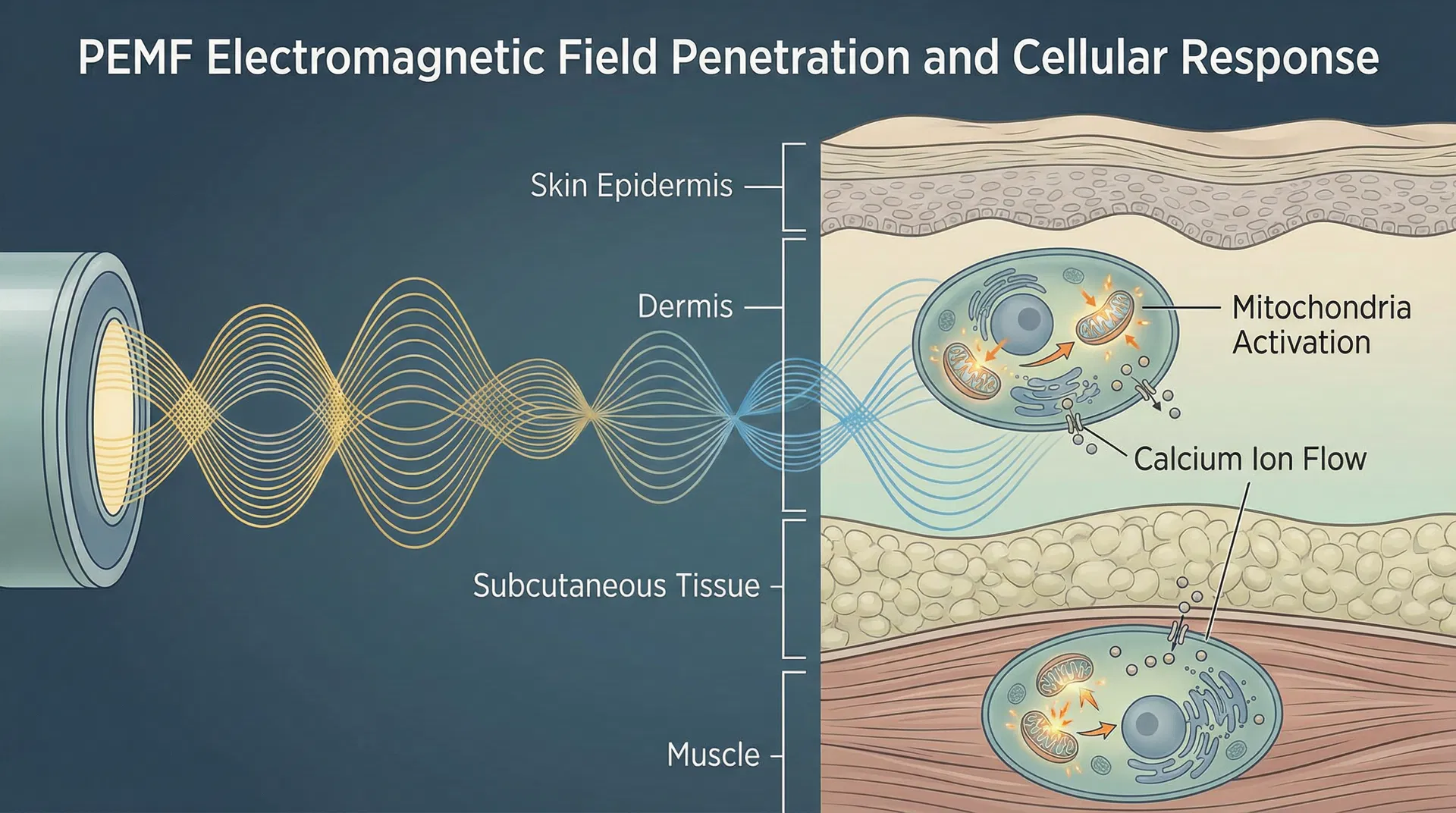
PEMF operates at the cellular level, using pulsed electromagnetic fields that penetrate tissue without requiring direct skin contact. Rather than forcing muscle contractions or blocking pain signals, PEMF works with the body's natural electromagnetic environment to activate cellular healing mechanisms. This distinction is not merely technical—it represents fundamentally different approaches to supporting recovery.
Cellular Mechanisms: How Each Modality Works
PEMF: Cellular-Level Activation
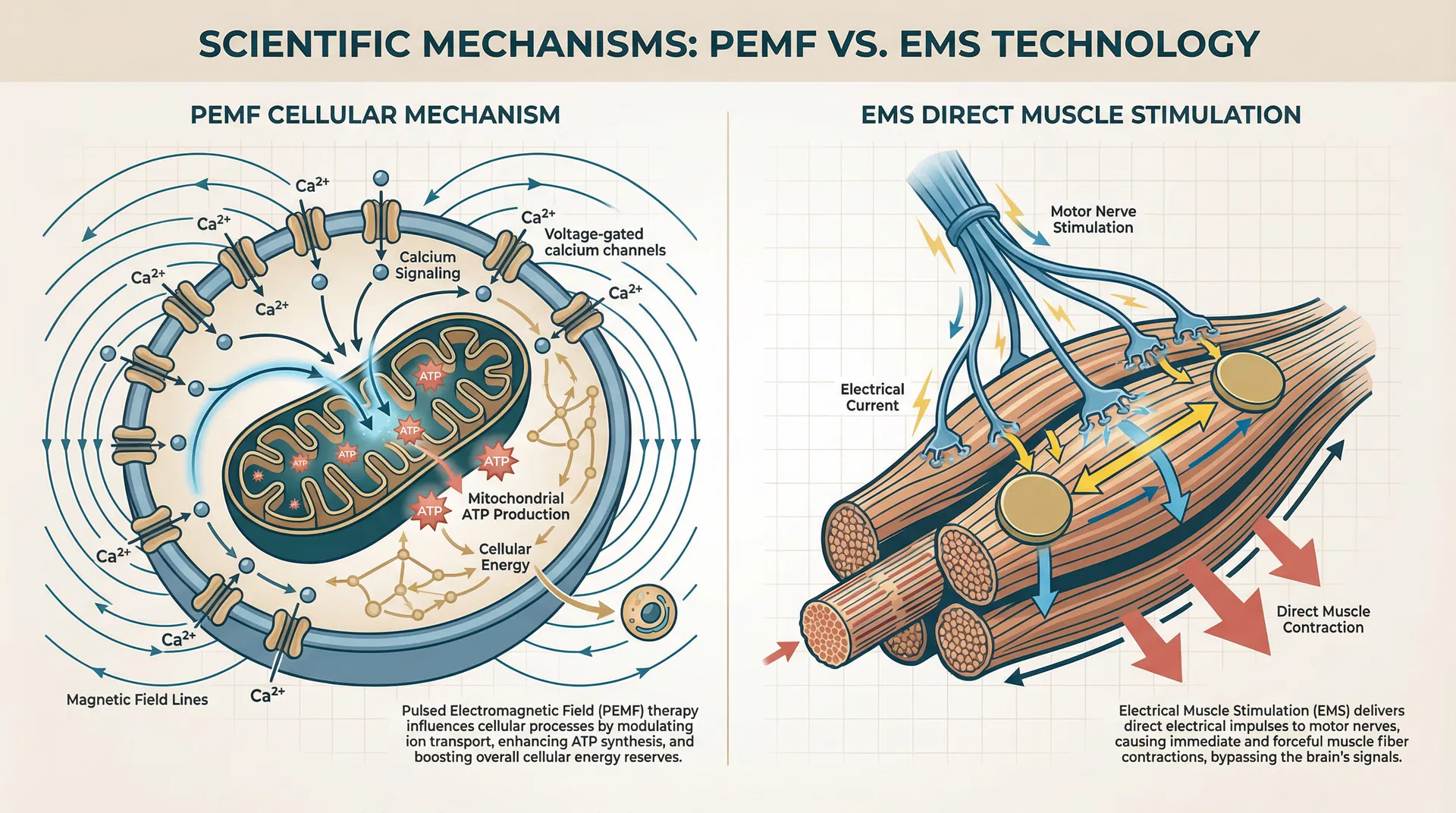
Pulsed electromagnetic field therapy activates specific cellular pathways that initiate healing from within. The mechanism centers on voltage-gated calcium channels (VGCCs) in cell membranes. When exposed to PEMF, these channels open, allowing calcium ions to flow into cells. This calcium influx triggers a cascade of beneficial cellular processes.
Within the mitochondria—the cell's energy-producing organelle—calcium signaling enhances ATP (adenosine triphosphate) production, the fundamental energy currency of cells. Increased ATP availability supports multiple recovery processes: muscle fiber repair, protein synthesis, inflammatory modulation, and tissue regeneration. Additionally, PEMF stimulates adenosine signaling through specific cell membrane receptors (A2A and A3), which promote protective cellular responses and tissue repair.
The beauty of this mechanism is its systemic nature. Because PEMF works at the cellular level through fundamental biological pathways, its benefits extend throughout treated tissues and even systemically, depending on the device and treatment area. Every cell type with the appropriate receptors can respond to PEMF stimulation, creating coordinated healing responses across multiple tissue systems.
EMS: Direct Muscle Fiber Activation
Electrical muscle stimulation works through a more direct pathway. Electrical current applied through electrodes penetrates tissue and stimulates motor nerves, causing involuntary muscle fiber contractions. These contractions generate force comparable to voluntary muscle contractions—typically around 30% of maximal voluntary contraction strength—making EMS effective for muscle training and strength development.
The mechanism is straightforward: electrical current depolarizes nerve fibers, triggering action potentials that propagate to muscle fibers, causing them to contract. Repeated contractions induce muscle fatigue, metabolic stress, and muscle damage markers (elevated creatine kinase activity and delayed-onset muscle soreness), which stimulate adaptation and strength gains through traditional exercise physiology pathways.
TENS: Nerve-Level Pain Modulation
TENS operates through the "gate-control theory" of pain. Electrical stimulation of sensory nerves creates competing sensory input that effectively "closes the gate" on pain signal transmission at the spinal cord level. This prevents pain signals from reaching the brain, providing rapid pain relief. However, this mechanism addresses pain perception rather than underlying tissue damage, making TENS primarily a symptomatic treatment.
Scope and Duration of Effects
The differences in mechanism translate directly into differences in scope and duration of therapeutic effects.
PEMF provides systemic, long-lasting benefits. Because it works at the cellular level through fundamental biological pathways, PEMF effects extend throughout the treated area and can include systemic benefits like improved circulation and reduced inflammation. Critically, these effects persist and accumulate over time. The cellular healing processes initiated by PEMF continue after treatment ends, creating lasting tissue regeneration and recovery benefits.
EMS provides localized, immediate but temporary effects. Muscle contractions occur only where electrodes are placed, and benefits are largely confined to that area. While immediate strength gains can occur during treatment, the effects diminish relatively quickly after stimulation ends. EMS is excellent for targeted muscle training but doesn't address systemic recovery or underlying tissue damage.
TENS provides rapid but fleeting pain relief. Pain reduction begins immediately upon application but typically subsides within minutes to hours after treatment ends. TENS is ideal for acute pain management but doesn't promote healing of the underlying cause of pain.
Clinical Evidence and Efficacy
Research demonstrates distinct efficacy profiles for each modality, reflecting their different mechanisms.
PEMF Research Findings
Clinical studies on PEMF therapy for muscle recovery show substantial benefits:
- Delayed-onset muscle soreness (DOMS) reduction: Research demonstrates 30-50% reduction in DOMS following intense exercise when combined with PEMF therapy, compared to control conditions [1]
- Accelerated strength recovery: Athletes using PEMF therapy show faster recovery of muscle strength and power output following intense training [1]
- Enhanced protein synthesis: PEMF stimulation increases muscle protein synthesis rates, supporting muscle repair and growth [1]
- Improved endurance capacity: Studies indicate enhanced endurance performance and faster recovery in endurance athletes [1]
- Pain management: PEMF therapy was significantly more effective at managing pain and reducing pharmacologic use than standard care treatment, with superior outcomes for pain, range of motion, functionality, and quality of life [2]
The consistency of these findings across diverse populations and conditions suggests that PEMF's cellular mechanism produces robust, reproducible benefits for muscle recovery and tissue healing.
EMS Research Findings
Electrical muscle stimulation has an extensive research history demonstrating its effectiveness for specific applications:
- Muscle strength development: EMS effectively increases muscle strength through training-induced adaptations, with force generation reaching approximately 30% of maximal voluntary contraction [3]
- Atrophy prevention: EMS is well-established for preventing muscle atrophy in immobilized or sedentary populations [3]
- Comparable acute responses: Research comparing alternating current and pulsed current EMS shows similar acute effects on muscle force, metabolic responses, and muscle damage markers [3]
- Rehabilitation applications: EMS supports rehabilitation following injury or surgery by maintaining muscle function during recovery periods [3]
EMS excels in applications requiring direct muscle activation and training stimulus but doesn't provide the cellular-level healing benefits of PEMF.
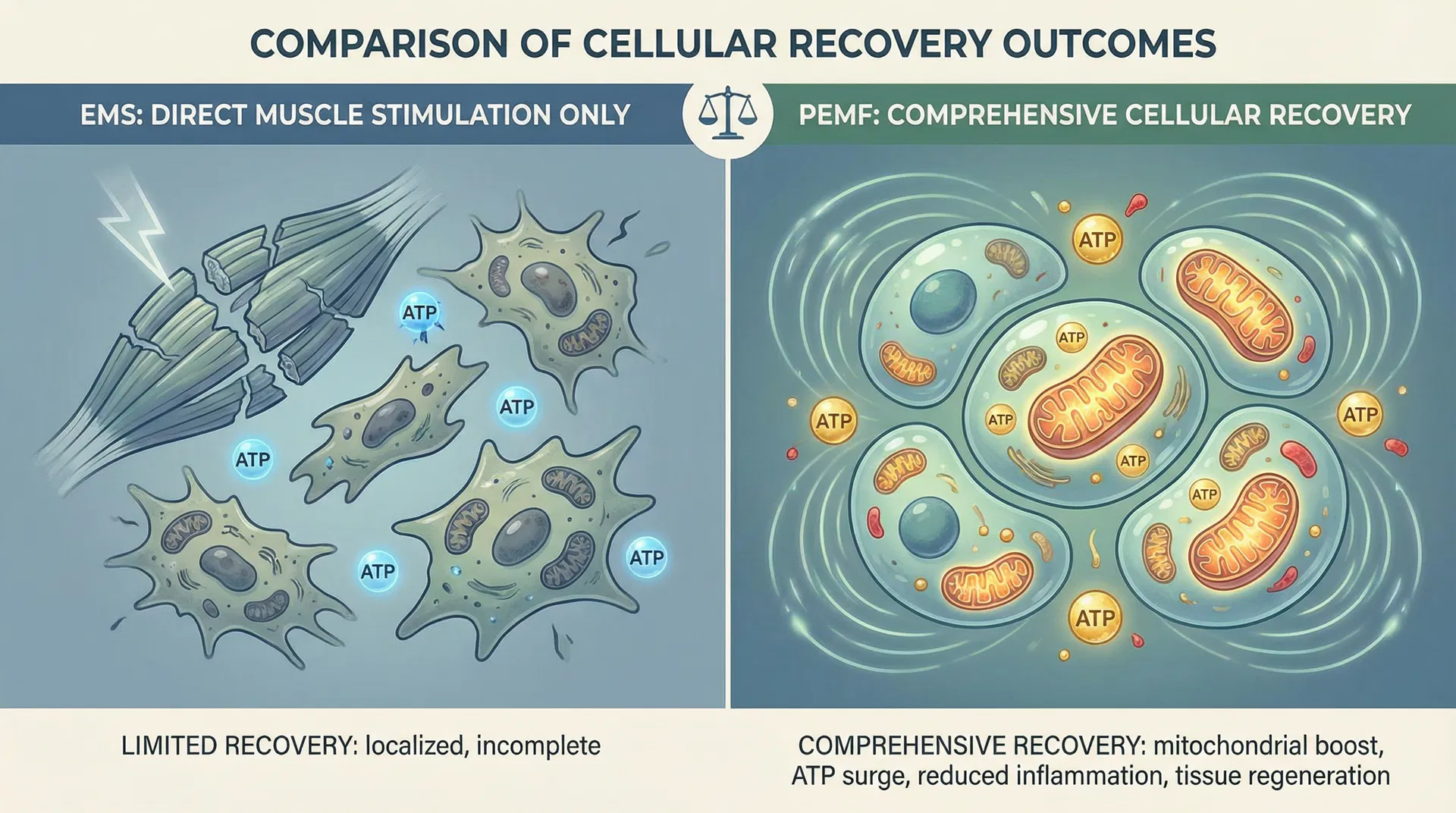
TENS Research Findings
TENS demonstrates clear effectiveness for pain management:
- Pain relief efficacy: TENS and PEMF show nearly equivalent effectiveness for specific pain conditions like post-herpetic neuralgia, though through different mechanisms [4]
- Rapid onset: Pain relief occurs immediately upon application, making TENS ideal for acute pain situations [4]
- Localized application: TENS effectively targets specific pain sites through direct electrode placement [4]
However, TENS doesn't address underlying tissue damage or provide lasting healing benefits beyond pain symptom management.
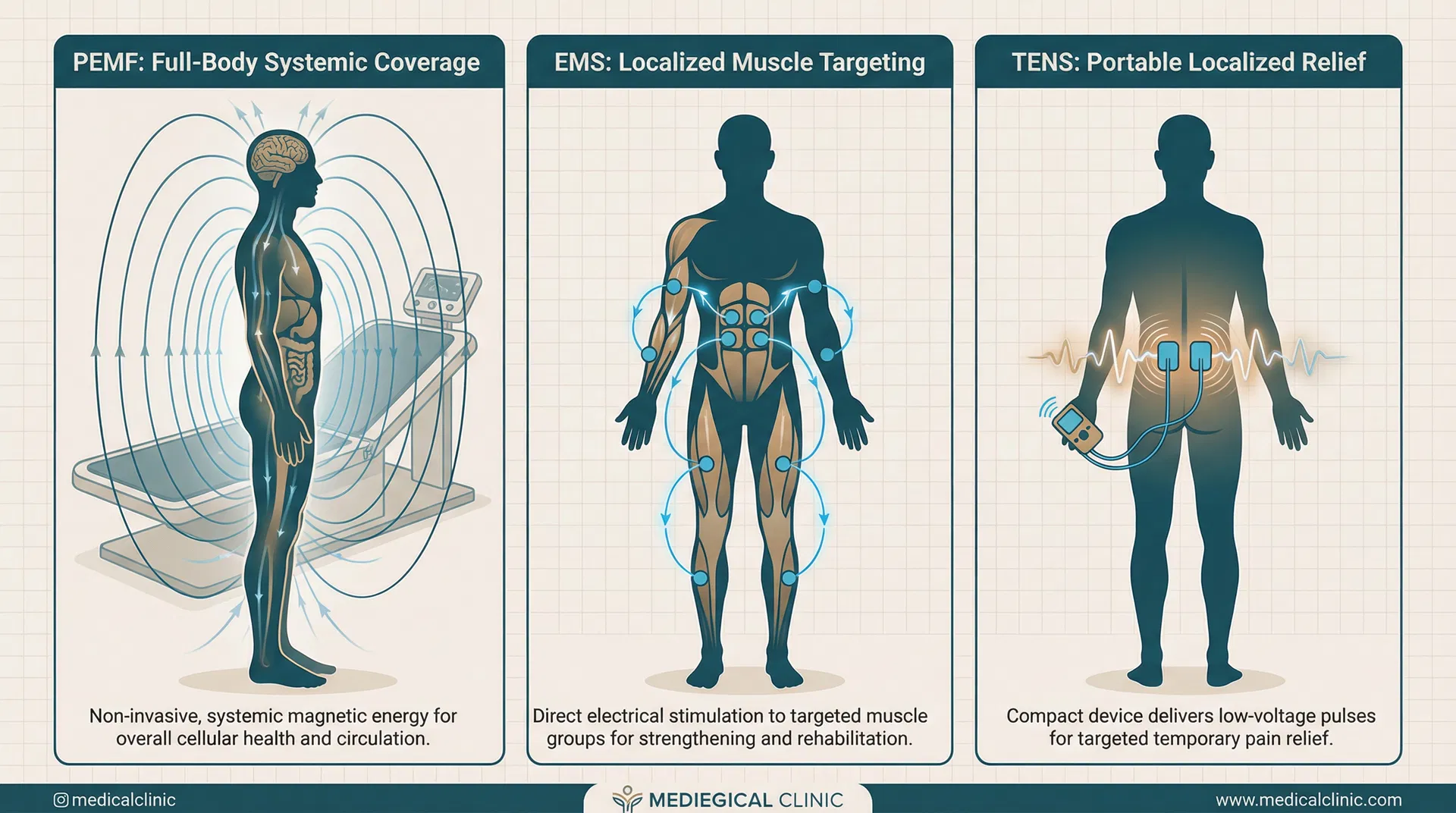
Practical Considerations: Application, Portability, and Cost
Beyond mechanism and efficacy, practical factors influence which modality suits different situations. PEMF typically requires a dedicated treatment space and offers full-body or large-area coverage with long-lasting benefits that accumulate over time. EMS provides moderate portability with handheld and wearable options, localized effects, and immediate but temporary results. TENS offers maximum portability with pocket-sized devices, localized application, and rapid but short-term pain relief.

Choosing the Right Modality for Your Goals
Selecting between PEMF, EMS, and TENS depends on your specific recovery objectives, timeline, and practical constraints.
Choose PEMF if you seek: Long-term tissue healing and regeneration, systemic recovery and anti-inflammatory benefits, cumulative improvements in recovery capacity, support for chronic conditions or deep tissue damage, or whole-body wellness and performance optimization.
Choose EMS if you seek: Targeted muscle strength development, localized muscle training and activation, prevention of muscle atrophy, rehabilitation support during recovery periods, or immediate muscle activation during treatment.
Choose TENS if you seek: Rapid, immediate pain relief, localized pain management, portable and convenient pain control, budget-friendly pain management options, or acute pain situations requiring quick relief.
The Complementary Nature of Different Modalities
Rather than viewing PEMF, EMS, and TENS as competing approaches, they can be understood as complementary tools serving different purposes within a comprehensive recovery strategy. An athlete might use TENS for immediate pain relief following an acute injury, EMS for targeted muscle activation during rehabilitation, and PEMF for long-term tissue healing and systemic recovery optimization.
The key distinction remains: PEMF addresses root causes through cellular healing, while EMS and TENS address symptoms or provide targeted training stimulus. For lasting recovery and performance enhancement, PEMF's cellular-level mechanism offers advantages that traditional electrical stimulation cannot provide.
Conclusion
The emergence of PEMF therapy represents a paradigm shift in how we approach muscle recovery and tissue healing. By working at the cellular level rather than simply stimulating nerves or muscles, PEMF activates the body's intrinsic healing mechanisms, producing lasting benefits that extend beyond the treatment session. While traditional electrical stimulation techniques like EMS and TENS remain valuable for specific applications—muscle training, pain relief, and rehabilitation support—PEMF offers a more comprehensive approach to supporting the body's natural recovery processes.
Understanding these distinctions empowers informed decisions about which recovery modality best serves your specific goals. For athletes and active individuals seeking optimal recovery and long-term tissue health, PEMF's scientifically-supported cellular mechanism offers a compelling complement to traditional training and rehabilitation approaches.
Ready to explore PEMF therapy for your recovery goals? Book Consultation with our Scottsdale specialists to discuss how PEMF can support your healing and wellness objectives.
Ready to explore this treatment?
Schedule Your ConsultationFrequently Asked Questions
How does PEMF differ from EMS and TENS?
PEMF works at the cellular level by activating calcium channels and enhancing mitochondrial ATP production, creating systemic and long-lasting healing effects. EMS directly stimulates muscle fibers through electrical current to produce contractions and immediate strength gains. TENS blocks pain signals at the nerve level for rapid but temporary pain relief. Each modality operates at a different biological level with distinct mechanisms and outcomes.
Which modality is best for muscle recovery?
PEMF is superior for comprehensive muscle recovery because it addresses root causes through cellular healing, reduces inflammation, enhances circulation, and supports tissue regeneration. EMS is excellent for targeted muscle training and strength development. TENS is best for immediate pain management. For optimal recovery, PEMF provides the most complete approach with lasting benefits.
How long do the effects of each modality last?
PEMF effects are long-lasting and cumulative, with benefits persisting and building over multiple sessions. EMS effects are immediate during treatment but diminish relatively quickly after stimulation ends. TENS provides rapid pain relief that typically subsides within minutes to hours after treatment. PEMF offers the most durable results for sustained recovery.
Can I combine PEMF, EMS, and TENS in a recovery program?
Yes, these modalities are complementary and can be strategically combined. You might use TENS for immediate acute pain relief, EMS for targeted muscle training during rehabilitation, and PEMF for long-term tissue healing and systemic recovery optimization. A comprehensive recovery strategy often benefits from using each modality for its specific strengths.
Is PEMF more expensive than EMS or TENS?
PEMF systems typically cost more initially ($500-$5,000+) compared to EMS ($100-$500) or TENS ($50-$200). However, PEMF's superior efficacy and long-lasting results often provide better overall value. When accounting for the total number of treatments needed to achieve comparable results, PEMF may be more cost-effective for comprehensive recovery and healing.